Description
Cerasorb M Key Benefits
- Alloplast Graft Gold Standard: Cerasorb M B-TCP with > 99% phase purity, has become the industry standard 1, cited in over 170 different publications.
- > 99% Resorption: resorption profile coincides with rate of bone formation, turning over to quality vital bone within 4-12 months.
- Unique Porosity: ~ 65% porosity, with full range of pore sizes and interconnected porosity, increasing osteoconductivity
- Osteoconductive: B-TCP particles provide optimal microenvironment for osteoblast adhesion and the capillary effect of the blood within the B-TCP granules promotes the rapid formation of osteoblasts which stimulates vital bone growth.
- Available in several granule sizes. Sold in Packs of 5 Vials per order.
Autograft is the gold standard for bone grafting, but can result in harvest site patient morbidity, and complications. For dental procedures where harvesting autograft isn’t feasible, an alternative is required that is easy to use and is effective. In many cases, you want to do more than just “repair” the problem—you want to regenerate the solution.
Cerasorb M provides maximum porosity for better resorption in bone grafting procedures. Made of a new generation of pure-phase ß-tricalcium phosphate, the product provides a unique interconnecting scaffolding that allows it to be completely resorbed while simultaneously creating new bone formation. as a result, it produces bone quality comparable to patients’ harvested bone, the gold standard for bone grafting techniques.
Cerasorb: Optimal Microenvironment
The technology built into CERASORB M is as easy as M-2-3. The M technology provides a full range of Micro, Meso and M acro pores (5-500 μm) in the uniquely polygonal shaped ß-TCP granules. This full range of interconnected pores allows deep cellular infiltration which leads to resorption, angiogenesis and ultimately bone remodeling.
Cerasorb: Predictable Bone Formation and Resorption
The capillary effect of the blood within the Cerasorb granules promotes the rapid formation of osteoblasts which stimulates vital bone growth. Cerasorb M with its consistent porosity and calcium phosphate ratio, similar to a patient’s own bone, provides predictable resorption and new bone formation in 4–6 months
CERASORB M is resorbed from both outer and inner pore surfaces, allowing resorption at the same rate of new bone formation.
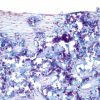
Different stages of absorption and remodeling Granule completely surrounded by lamellar bone tissue (letters below reference the image to the right)
- Osteoclasts starting the resorption process along outside margin of granule
- Resorption from inside to outside: osteoblast bone-building activity within center of granule
- Resorption from outside to inside: central building of osteons
- New bone formation, containing osteocytes, throughout former defect site with no fibrous tissue formation. Residual CERASORB fragments remain, with osteoblasts still actively mineralizing the margins.
(Prof. Plenk, Dr. Lederer, Vienna)
Cerasorb: Backed by Years of Research
CERASORB is a well-studied biosynthetic. With over 170 different publications, ranging from pre-clinical studies to human clinical results, curasan provides research results that are second to none. CERASORB M sets the standard for alloplasts
- In studies of a variety of scaffold types, the CERASORB scaffold provided a better surface for osteoblast proliferation. 2,3
- 10 year comparative study in which implantation in extraction alveoli augmented with CERASORB proved equal to implantation in natural bone.4
- In a bilateral sinus lift study, results suggest CERASORB is an equivalent graft material to autogenous bone.5
- Handling, efficacy and healing of the bone substitute were generally rated as “very good” or “good” and yielded a rate of 90% for both efficacy and tolerance.6
- Twenty-two patients with contralateral intrabony defects were treated with β-TCP CERASORB® alone or in combination with PRP. β-TCP CERASORB is a satisfactory graft material in periodontal surgery, even without PRP. 7
1. ICDD (International Center for Diffraction Data, Pennsylvania, USA) reference standards since 2005.
2. XTT-Colormetrietest aus der Habilitationschrift von Dr. med. dent. Murat Yildirim, RWTH Aachen, 2002
3. Bernhardt A, Lode A, Peters F, Gelinsky M. Novel ceramic bonereplacementmaterial Osbones in a comparative invitro study with osteoblasts. Clin. Oral Impl. Res. 22, 2011; 651–657.
4. Harel, N., et al. (2013): Long-term Results of Implants Immediately Placed into Extraction Sockets Grafted with ß-TCP: A Retrospective Study. J Oral Maxillofac Surgery 2013, 71(2): e63-e68
5. Szabo G, Huys, et al. International Journal of Oral and Maxillofac Implants 2005; 20:371-381.
6. Bilk, Dieter. (2007); CERASORB M in Dental Surgery: Post-Marketing Surveillance Study with 148 patients. EDI Journal 2007; 4: 40-46
7. Harnack L, et al, (2009) Use of platelet-rich plasma in periodontal surgery—a prospective randomised double blind clinical trial. Clin Oral Investig. 2009 Jun: 13 (2): 179-187.




Reviews
There are no reviews yet.